A grace period in medical billing is a temporary timeframe after an insurance premium payment is missed during which a patient’s health coverage may remain active. During this period, claims can be delayed, suspended, or denied depending on the payer and the stage of the grace period. Medical billing teams must verify eligibility carefully to reduce reimbursement risk and prevent avoidable denials.
What Is a Grace Period in Medical Billing?
A grace period in medical billing is the amount of time a health insurance company allows a policyholder to make overdue premium payments before coverage is terminated.
In healthcare revenue cycle management, grace periods are important because they directly affect:
- insurance eligibility,
- claim reimbursement,
- denial management,
- and patient financial responsibility.
For providers and billing teams, a patient may appear insured during part of the grace period even though the payer has not received premium payments. That can create reimbursement uncertainty if services are rendered before coverage officially lapses.
Why Insurance Grace Periods Matter in Revenue Cycle Management
Insurance eligibility verification is one of the earliest steps in the medical billing workflow. If a patient enters a grace period due to unpaid premiums, the provider’s reimbursement risk increases.
A grace period can affect:
- Claim approval timing
- Payment posting
- Prior authorization validity
- Patient collections
- Denial management workflows
For example, a clinic may submit a claim through a clearinghouse only to discover the payer has placed the claim in a pending status because the patient is behind on premium payments.
This is why many practices integrate real-time eligibility checks into their EHR or practice management systems before appointments.
Healthcare organizations that already follow structured workflows outlined in a “Medical Billing Process Guide” typically experience fewer avoidable reimbursement delays.
How the ACA Grace Period Works
Under the Affordable Care Act (ACA), some marketplace insurance plans provide a 90-day grace period for members receiving premium subsidies.
The grace period is generally divided into stages:
First 30 Days
The insurer usually continues paying claims normally if coverage was previously active.
Providers may not immediately notice a payment issue during this phase.
Days 31–90
Claims may be:
- suspended,
- pended,
- or denied later if premiums remain unpaid.
This creates financial risk for healthcare providers because services may already have been delivered before final coverage determination occurs.
Approximate insight based on industry patterns: many provider organizations increase eligibility verification frequency during this period to reduce exposure to unpaid claims.
After the Grace Period Ends
If premiums remain unpaid, insurers may terminate coverage retroactively to the end of the first grace period month.
At that point:
- denied claims may become patient responsibility,
- appeals may increase,
- and collection workflows become more complex.
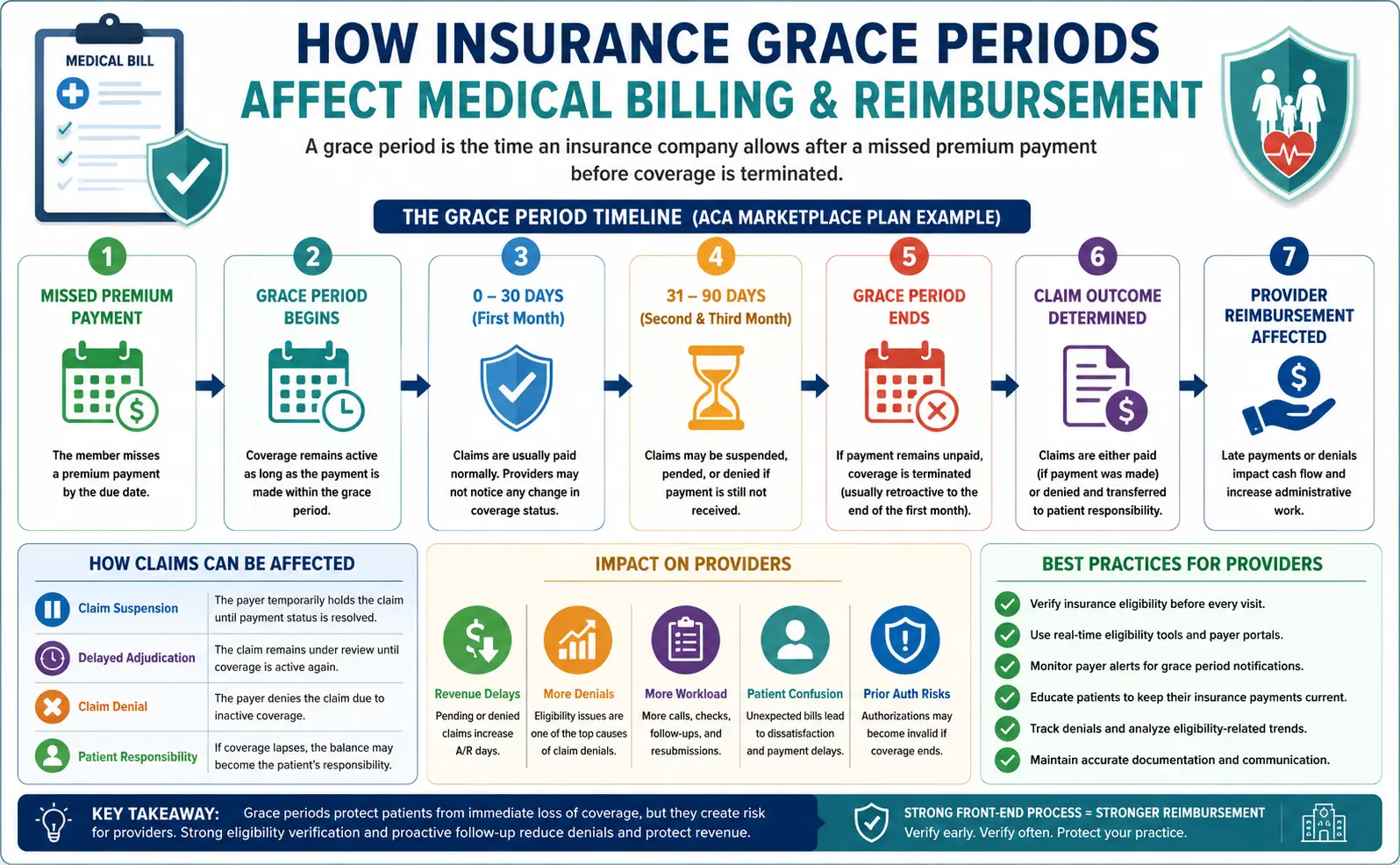
What Happens to Medical Claims During a Grace Period
Claims behavior varies by payer, plan type, and policy rules.
Common scenarios include:
Claim Suspension
The payer temporarily holds the claim pending premium payment status.
Claim Denial
The insurer denies reimbursement because coverage became inactive.
Delayed Adjudication
The claim remains under review until eligibility status is finalized.
Patient Balance Transfer
The provider may need to transfer financial responsibility to the patient if coverage lapses.
This is closely connected to denial prevention and reimbursement workflows discussed in broader “How Denial Management Works” content.
Common Billing Risks for Providers
Grace periods create several operational risks inside healthcare billing departments.
Revenue Delays
Pending claims can slow cash flow and increase accounts receivable days.
Increased Denials
Claims submitted during inactive coverage periods often trigger eligibility-related denials.
Administrative Burden
Billing teams may spend additional time:
- checking payer portals,
- contacting insurance representatives,
- resubmitting claims,
- or managing patient statements.
Prior Authorization Complications
Even approved prior authorizations may become problematic if coverage terminates during treatment.
Patient Satisfaction Issues
Patients are often unaware they entered a grace period, creating confusion when balances appear unexpectedly.
How Medical Billers Reduce Grace Period Denials
Strong front-end revenue cycle processes are critical.
Verify Insurance Before Every Visit
Eligibility checks should occur:
- during scheduling,
- before appointments,
- and again before claim submission when possible.
Many practices use automated clearinghouse tools integrated into EHR/EMR systems.
Monitor Payer Alerts
Some insurers notify providers when patients enter grace periods.
Billing staff should document these alerts carefully while maintaining compliance with HIPAA privacy requirements.
Educate Patients Early
Front-desk staff can encourage patients to confirm insurance payment status before services are rendered.
Strengthen Denial Tracking
Practices with structured denial management programs can identify recurring eligibility denial patterns faster.
This connects naturally with broader educational resources like:
- “Insurance Claim Submission Process”
- “Medical Coding vs Medical Billing”
- “What Is Revenue Cycle Management”
Maintain Accurate Documentation
Accurate ICD-10 and CPT coding remains essential even when eligibility issues occur because claims may later be reprocessed after premium payment resolution.
Best Practices for Healthcare Organizations
Healthcare organizations can reduce grace period exposure by building stronger insurance verification protocols into daily operations.
Recommended best practices include:
Use Real-Time Eligibility Verification
Automated eligibility tools reduce manual verification errors.
Create High-Risk Claim Workflows
Flag claims involving:
- marketplace plans,
- recurring eligibility issues,
- or prior payment delays.
Train Front-End Staff
Scheduling and registration teams should understand how grace periods affect reimbursement.
Improve Communication Between Departments
Clinical, billing, and patient access teams should share insurance status updates promptly.
Audit Denial Trends
Regular denial audits help practices identify payer-specific grace period risks.
Organizations focused on proactive revenue cycle management often experience lower preventable denial rates and more stable reimbursement performance.

How long is a grace period in medical billing?
The length varies by insurer and plan type. ACA marketplace plans with premium subsidies commonly allow a 90-day grace period.
Can insurance deny claims during a grace period?
Yes. Some claims may be suspended or denied if premiums remain unpaid during later stages of the grace period.
Are providers notified when a patient enters a grace period?
Some payers notify providers through eligibility systems or payer portals, but notification practices vary.
Who becomes financially responsible if coverage lapses?
If insurance coverage terminates, the patient may become responsible for unpaid balances depending on payer policies and provider agreements.
Why is eligibility verification important during a grace period?
Eligibility verification helps providers reduce reimbursement risk, prevent denials, and identify inactive coverage before services are rendered.













