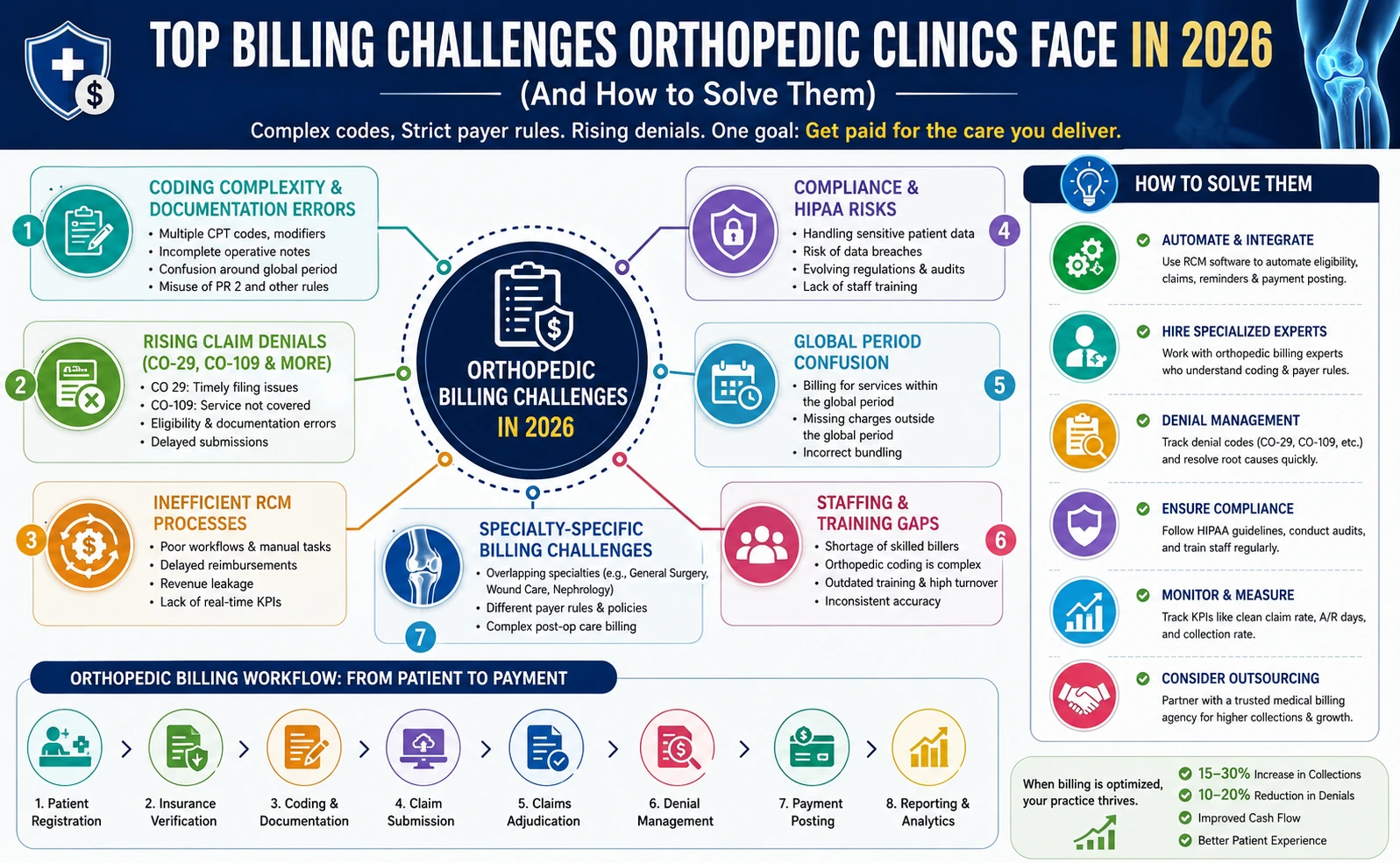
Billing Challenges Orthopedic clinics in 2026 struggle with complex coding, rising claim denials, evolving compliance rules, and inefficient revenue cycle management (RCM). Solving these requires better automation, specialized billing expertise, denial tracking, and proactive audits. Clinics that optimize billing workflows can increase revenue by 15–30%.
If you’re running or managing an orthopedic clinic in 2026, you already know this: billing is no longer just an administrative task—it’s a revenue battlefield.
Orthopedic billing involves high-value procedures, strict payer rules, and intricate coding systems. A small error can cost thousands. Many clinics still rely on outdated workflows, which leads to denied claims, compliance risks, and lost revenue.
This guide breaks down the top billing challenges orthopedic clinics face in 2026—and more importantly, how to fix them.
Why Orthopedic Billing Is More Complex Than Ever
Orthopedic practices deal with:
- High-cost surgeries (joint replacements, spine procedures)
- Multiple modifiers and CPT codes
- Strict payer-specific rules
- Long global periods after surgery
Add to that evolving compliance standards and insurance scrutiny—and billing becomes a serious operational challenge.
Top Billing Challenges Orthopedic Clinics Face in 2026
1. Coding Complexity & Documentation Errors
Orthopedic procedures require highly specific coding. Mistakes often occur due to:
- Incorrect modifiers
- Misuse of PR 2 in medical billing scenarios (patient responsibility issues)
- Incomplete operative notes
Even experienced billers struggle because orthopedic coding evolves constantly.
Related challenges:
- Confusion around what is global period in medical billing
- Misinterpretation of procedure bundling rules
Solution:
Invest in specialty-trained coders and conduct regular medical billing audit services.
2. Rising Claim Denials (CO-29, CO-109, and More)
Denials are one of the biggest financial drains.
Common denial codes include:
- CO 29 denial code descriptions – timely filing issues
- CO-109 denial code description – service not covered
These are often preventable but occur due to:
- Incorrect patient eligibility verification
- Delayed submissions
- Missing documentation
Impact:
Clinics lose 10–20% of revenue due to avoidable denials.
Solution:
Implement denial tracking systems and proactive resubmission workflows.
3. Inefficient RCM (Revenue Cycle Management)
Many clinics still ask: what is RCM in medical billing?
RCM includes:
- Patient registration
- Coding
- Claims submission
- Payment posting
- Denial management
Poor RCM leads to:
- Delayed reimbursements
- Revenue leakage
- Increased administrative costs
Solution:
Automate workflows and consider outsourcing to a medical billing agency Delaware or specialized providers.
4. Compliance & HIPAA Risks
With stricter regulations, compliance errors can result in heavy penalties.
A common question is:
why is HIPAA important for billing and coding?
Because billing involves:
- Patient data
- Insurance details
- Treatment records
Any breach can lead to legal consequences.
Solution:
- Regular compliance audits
- Staff training
- Secure billing systems
5. Global Period Confusion
Orthopedic surgeries often include a global period, meaning follow-up care is bundled into the original payment.
Errors happen when clinics:
- Bill separately for included services
- Fail to bill eligible services outside the global period
Result:
Denied claims and lost revenue.
6. Specialty-Specific Billing Challenges
Orthopedic clinics often overlap with other specialties, creating additional complexity:
- general surgery medical billing overlaps in trauma cases
- wound care billing services for post-surgical care
- gastroenterology billing services in related procedures
Each specialty has different payer rules.
7. Staffing & Training Gaps
Many clinics face shortages of skilled billers.
Common concerns include:
- is medical billing and coding hard? → Yes, especially for orthopedics
- is medical billing and coding worth it? → Only with specialization
Some clinics rely on inexperienced staff or outdated training programs (e.g., mixed reviews like devry university medical billing and coding reviews).

Comparison: In-House vs Outsourced Billing
| Feature | In-House Billing | Outsourced Billing |
|---|---|---|
| Cost | High (staff + training) | Predictable monthly fee |
| Expertise | Limited | Specialized teams |
| Denial Rate | Higher | Lower |
| Compliance | Risky | Managed by experts |
| Scalability | Difficult | Easy |
Real-World Case Study
A mid-sized orthopedic clinic in 2025 faced:
- 22% claim denial rate
- Delayed reimbursements (45+ days)
After switching to a specialized billing provider:
- Denials reduced to 8%
- Revenue increased by 27%
- Billing turnaround improved by 35%
Expert Tips to Improve Orthopedic Billing in 2026
- Use automation tools for eligibility checks
- Invest in medical billing consultation
- Conduct quarterly audits via a medical billing audit company
- Train staff in specialty coding
- Track denial codes aggressively
- Stay updated with medical billing news today
1. What is the biggest challenge in orthopedic billing?
Coding complexity and high denial rates are the biggest issues.
2. What happens to medical bills when you die?
They are typically paid from the estate, not inherited directly by family members (laws vary).
3. What is an entity code in medical billing?
It identifies the type of provider or organization involved in a claim.
4. Can you go to jail for not paying medical bills?
No, unpaid medical bills are civil matters, not criminal offenses.
5. What are medical billing responsibilities?
They include coding, claims submission, payment posting, and denial management.
6. How do audits improve billing performance?
They identify errors, reduce denials, and improve compliance.
7. Which specialties have similar billing complexity?
Nephrology, cardiology, dermatology, and podiatry billing share similar challenges.













