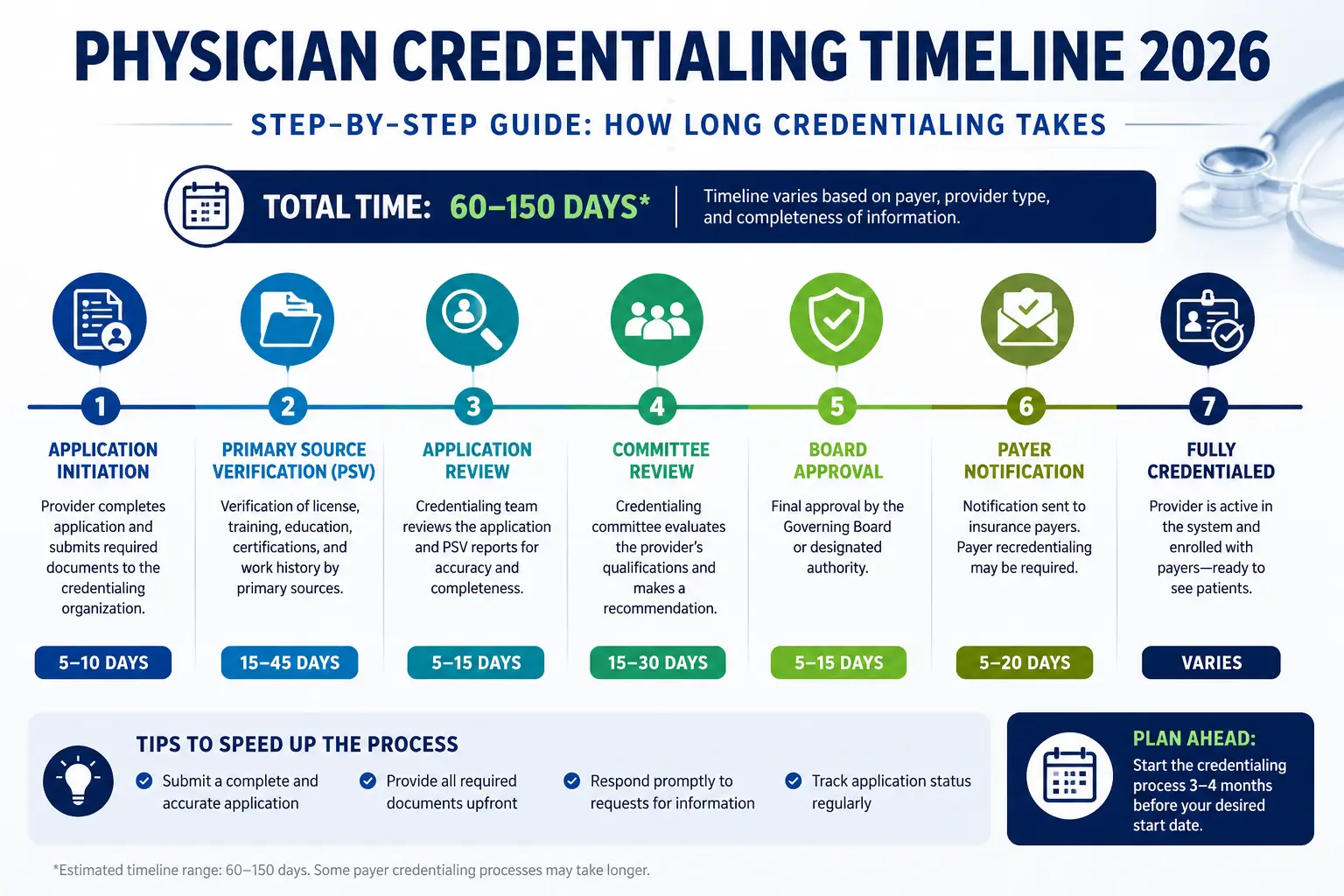
Physician Credentialing 2026: 8 Steps, Real Timelines & How to Avoid Costly Delays
You just hired a great new doctor. She is ready to see patients on Monday. Your schedule is filling up. Revenue is waiting.
Then someone mentions credentialing.
Suddenly Monday becomes March.
If you have ever watched a new provider sit idle for months because insurance companies have not finished their paperwork — you already know exactly how painful the physician credentialing process can be. And if you are opening a new practice or bringing on your first provider, you are about to find out.
This guide covers everything: what credentialing actually is, the 8 real steps it takes, how long each payer takes in 2026, and — most importantly — what you can do right now to speed up the process and protect your revenue while you wait.
What Is Physician Credentialing? (The Plain-English Version)
Physician credentialing is the formal process through which insurance companies, hospitals, and healthcare organizations verify that a provider is who they say they are — and that they are qualified to treat patients and receive payment for their services.
Before a doctor can bill Medicare, Medicaid, or any private insurance plan, that payer needs to confirm:
- Where the doctor went to medical school
- Whether their license is valid and in good standing
- Whether they have active malpractice insurance
- Whether they have any disciplinary history, sanctions, or malpractice claims
- What specialties and procedures they are trained to perform
None of this is optional. A provider who sees patients before credentialing is complete cannot legally collect reimbursement from most payers for those visits. That is not a technicality — it is real money your practice will never recover.
Simple version for anyone: Credentialing is like a background check combined with a job application — except the employer is every insurance company you want to work with, and each one has its own forms, its own process, and its own timeline.
It is worth noting that credentialing and provider enrollment are related but different:
- Credentialing = verifying qualifications
- Provider enrollment = officially registering with a payer to bill them
- Contracting = agreeing on the payment rates
All three must happen before the first clean claim goes out.
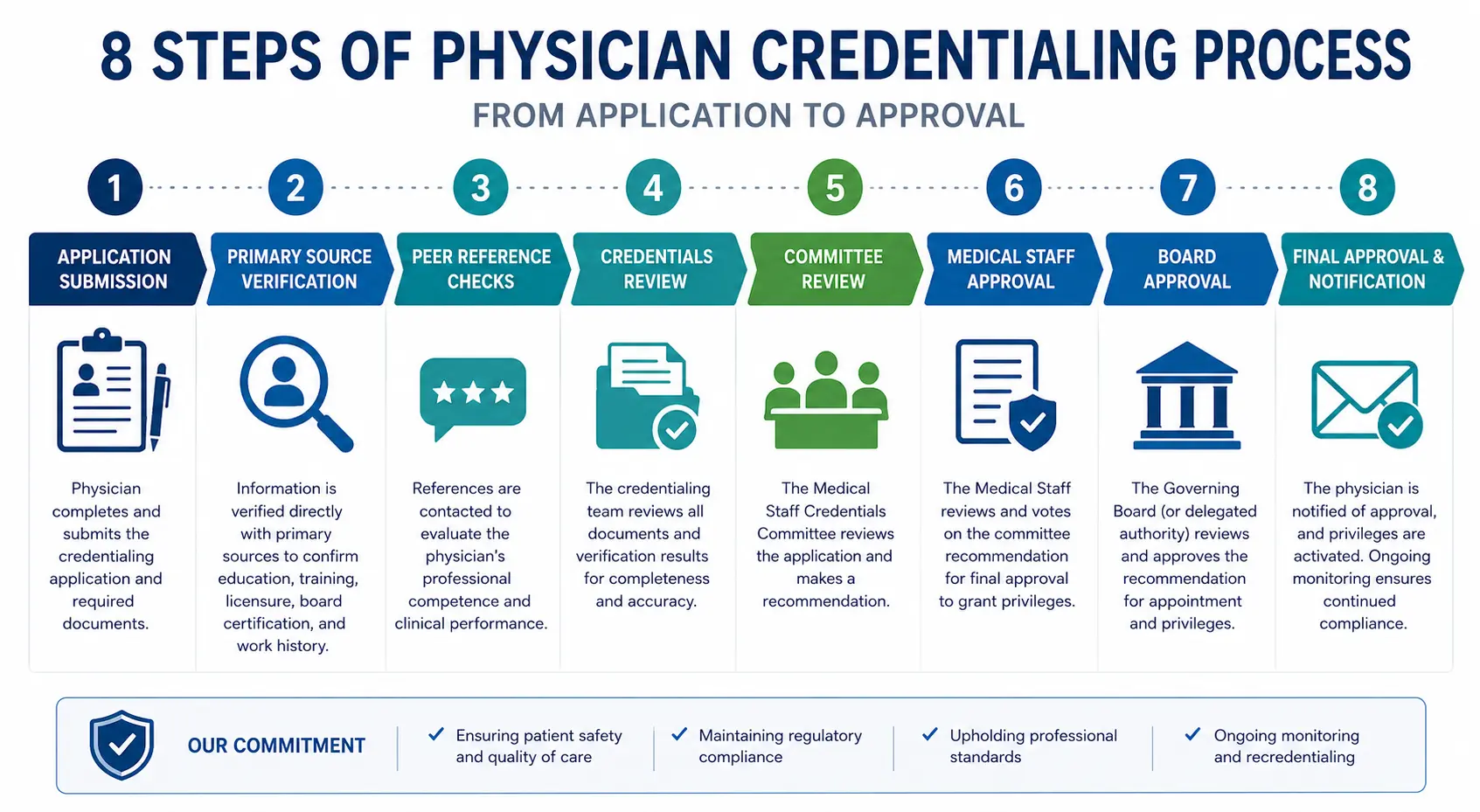
The 8 Steps of Physician Credentialing — What Actually Happens
Most people hear “credentialing takes 90 days” and imagine 90 days of waiting. In reality, those 90 days are a sequence of specific steps. Skip a step, miss a deadline, or submit one wrong document — and you are not just delayed. You are sent to the back of the line.
Here is exactly what happens, in order.
Step 1: Gather All Required Documents (Week 1–2)
This is the step that trips up most practices. Before you submit a single application, you need to have every document collected, verified, and organized. Missing even one item from this list causes delays of weeks — not days.
Documents required for every credentialing application:
- Current medical license (all states where provider will practice)
- DEA registration certificate
- National Provider Identifier (NPI) — Type 1 individual
- Board certification certificate (if applicable)
- Medical school diploma
- Residency and fellowship completion letters
- Complete work history with no gaps unexplained
- Malpractice insurance certificate with coverage dates and amounts
- Curriculum vitae (CV) — updated within 6 months
- References from 3–5 peers
- Professional liability history — all malpractice claims and outcomes
- CAQH ProView profile — complete and attested within the last 120 days
- DEA controlled substance registration
- Medicare and Medicaid provider numbers (if existing provider)
- Any state-specific documents required by each payer
Pro tip: Create a master credentialing folder — physical or digital — that holds every one of these documents. When you update one (like a license renewal), update it everywhere simultaneously. One outdated document in one application can cause a delay at any point in the process.
Step 2: Complete and Update Your CAQH ProView Profile (Week 2–3)
CAQH ProView is the centralized database that over 2.5 million healthcare providers use to store their credentialing information. More than 1,000 health plans use CAQH as their primary data source when reviewing applications.
If your CAQH profile is outdated, incomplete, or has expired attestation — every payer that pulls from it will get wrong information. That creates delays across all applications simultaneously.
CAQH rules you must follow:
- You must re-attest your CAQH profile every 120 days — without exception
- All information must match exactly what is in your license and certification documents
- Upload actual document scans — not just typed information
- Set a calendar reminder for Day 110 of every 120-day cycle
If you are setting up a CAQH profile for the first time, budget 3–5 business days to complete it thoroughly. Rushing this step costs far more time later.
Step 3: Obtain or Verify State Medical Licensure (Week 1–6, Parallel)
Every state where a provider will see patients requires a separate medical license. State licensing timelines vary enormously:
| State | Typical Licensing Timeline |
|---|---|
| Georgia | 4–8 weeks |
| Florida | 6–10 weeks |
| California | 8–16 weeks |
| Texas | 8–12 weeks |
| New York | 10–20 weeks |
| Illinois | 8–14 weeks |
Important 2026 update: The Interstate Medical Licensure Compact (IMLC) now includes 42 states plus Washington D.C. and Guam. If your provider holds a license in a Compact member state, they can get expedited licenses in other member states in 14–21 days — a massive time saver for providers practicing across multiple states or offering telehealth.
Start the licensing process the moment you know a provider is joining your practice. Do not wait until other paperwork is done.
Step 4: Apply to Medicare via PECOS (Week 3–4)
If your practice accepts Medicare — and most practices do — the provider must enroll through PECOS (Provider Enrollment, Chain, and Ownership System), which is CMS’s official online enrollment portal.
2026 Medicare credentialing timelines:
- Electronic PECOS submission with no site visit: 15–30 days
- Electronic PECOS submission requiring site visit: 45–65 days
- Paper application: 45–90 days (avoid paper whenever possible)
Electronic submissions process significantly faster than paper. There is almost never a reason to submit a paper Medicare application in 2026.
Common PECOS mistakes that cause delays:
- NPI number entered incorrectly
- Practice address does not match state license address
- Reassignment of benefits not completed
- Missing or expired Medicare Participating Provider agreement
- Ownership information incomplete for group practices
Step 5: Submit Medicaid Enrollment Applications (Week 3–4, Parallel)
Medicaid credentialing is handled state by state, and the timelines are the most unpredictable of any payer category. Federal rules require states to process applications within 45–90 days, but many states consistently miss this standard.
State Medicaid timeline examples in 2026:
| State | Medicaid Timeline |
|---|---|
| Georgia | 60–90 days |
| Florida | 45–90 days |
| Texas | 60–120 days |
| California | 60–90 days |
| New York | 90–180 days |
| Illinois | 60–120 days |
| Nebraska | 45–75 days |
| Arizona | 45–90 days |
| Colorado | 60–90 days |
| Idaho | 45–75 days |
If your practice serves a significant Medicaid population, submit Medicaid applications at the same time as Medicare — not after.
Step 6: Apply to Commercial Insurance Networks (Week 4–6)
This is often the slowest part of the entire credentialing process. Commercial payers — Blue Cross Blue Shield, Aetna, UnitedHealthcare, Cigna, Humana, and others — each have their own application portals, their own document requirements, and their own internal review committees that may only meet monthly.
Commercial payer timeline ranges in 2026:
| Payer | Typical Timeline |
|---|---|
| Blue Cross Blue Shield | 60–120 days |
| UnitedHealthcare | 90–150 days |
| Aetna | 90–120 days |
| Cigna | 90–150 days |
| Humana | 90–120 days |
| Medicaid Managed Care Plans | 90–180 days |
Critical fact: Some commercial payer networks are closed to new providers in certain specialties or geographic areas. Before investing weeks in an application, verify that the payer’s network is open in your area for your specialty.
Step 7: Primary Source Verification (Ongoing, Weeks 4–10)
While applications are processing, each payer independently verifies your provider’s credentials directly from the original sources — not from documents you submitted. They contact:
- Medical schools to confirm graduation
- Residency programs to confirm completion
- State medical boards to confirm license status
- The National Practitioner Data Bank (NPDB) for malpractice and disciplinary history
- Board certification bodies to confirm specialty credentials
- Previous employers to confirm work history
- Malpractice carriers to confirm coverage
This step is largely outside your control — but delays happen when your submitted information does not exactly match what primary sources report. Even small discrepancies, like a middle name shortened or a graduation date off by one month, create back-and-forth that adds weeks to the timeline.
2026 important change: NCQA now requires healthcare organizations to verify provider credentials every 30 days instead of the previous 6-month cycle. This applies to all credentialing files processed after July 1, 2025. Make sure your credentialing tracking system can handle monthly monitoring.
Step 8: Committee Review, Approval & EFT Setup (Weeks 10–16)
The final step before a provider can bill involves internal committee review at each payer, which may only happen once a month. After approval:
- You receive an effective date — the date from which claims can be submitted
- Contracts are executed (for commercial payers)
- You set up Electronic Fund Transfer (EFT) to receive payments directly
- You confirm billing information in each payer’s system
Do not skip the EFT setup. Practices that receive paper checks instead of electronic payments lose processing time and create unnecessary administrative work on every payment cycle.
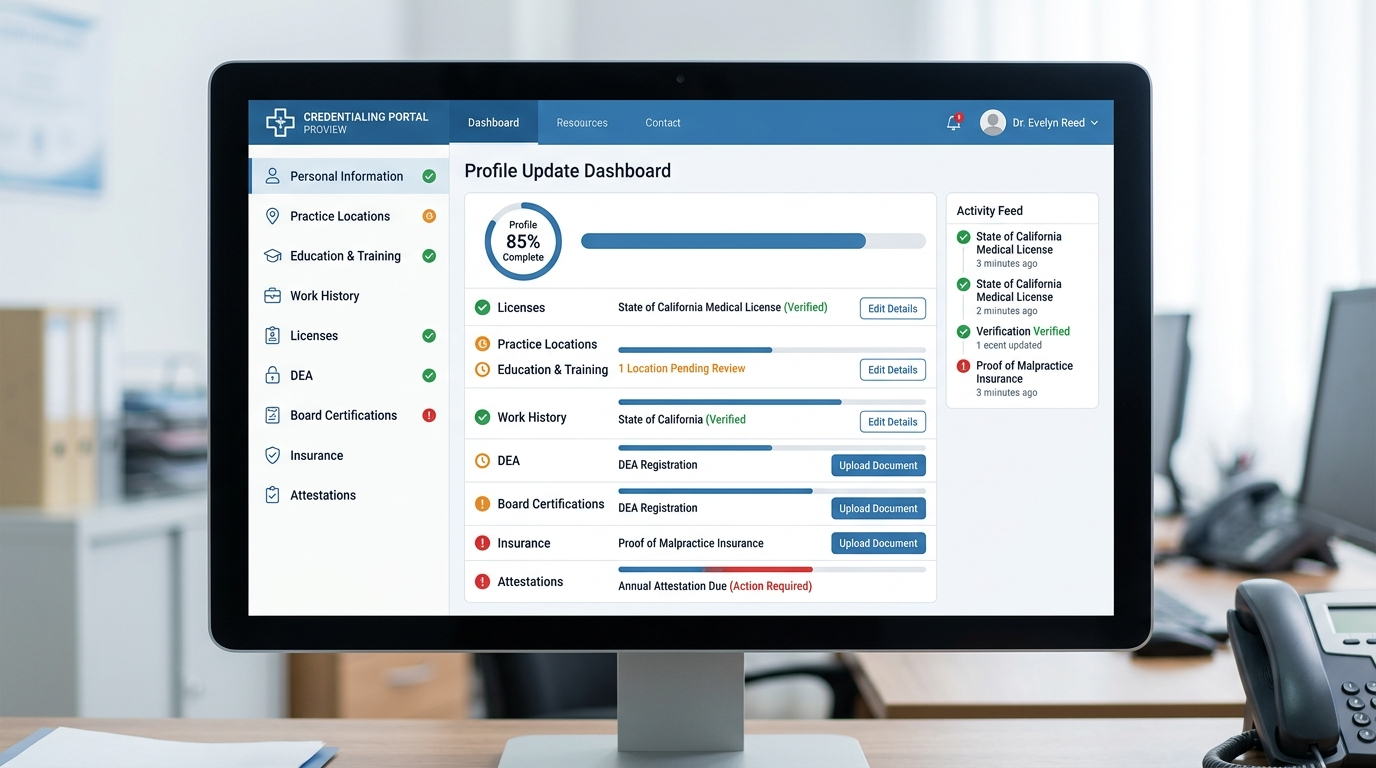
How Long Does Physician Credentialing Really Take in 2026?
Here is the honest answer that nobody else gives you:
The “90-day” number everyone quotes is technically true — and practically misleading.
The actual range in 2026 is 60 to 180 days, depending on:
- Which payers you are applying to
- Which state(s) the provider will practice in
- How complete and accurate the initial application is
- Whether CAQH is up to date before you start
- Whether you are applying during peak onboarding seasons (January and July are the slowest months)
- Whether the provider has a complex background, multiple state licenses, or malpractice history
The real financial impact of credentialing delays:
Research from the credentialing industry shows that physicians contribute an average of $200,000 to $300,000 in revenue per month to a practice. Every month of credentialing delay is a month of that revenue either lost or delayed.
For a small practice bringing on a new provider at $250,000 per month in revenue contribution, a 4-month credentialing delay instead of a 2-month delay costs approximately $500,000 in unrealized revenue.
That number is why experienced practice managers start credentialing 120 days before a provider’s intended start date — not 60 days, not 30 days. 120 days.
The 9 Most Common Causes of Credentialing Delays — And How to Avoid Each One
Every delay in credentialing has a cause. Most of them are preventable. Here are the nine we see most often.
1. Incomplete CAQH Profile
If CAQH is missing documents or has expired attestation, every payer that pulls from it gets bad data. Fix: Update CAQH before submitting any applications, and set a 110-day recurring reminder to re-attest.
2. Missing or Expired Documents
A license that expired last month, malpractice coverage with a gap, or a CV that has not been updated in two years — any of these stop an application cold. Fix: Build a master document checklist and audit it before submission.
3. Discrepancies Between Documents
Your provider’s name appears as “Robert” on their medical school diploma but “Bob” on their application. Their residency completion date is listed as June 30 but the program confirms July 1. These small mismatches trigger manual review that adds weeks. Fix: Cross-check every document against every other document before submitting.
4. Not Starting Early Enough
Starting credentialing 60 days before a provider’s start date almost guarantees a gap where the provider cannot bill. Fix: Start 120 days before the intended start date, minimum.
5. Submitting Paper Applications
Paper applications move to the back of every payer’s processing queue. In 2026, there is almost no reason to submit paper. Fix: Use PECOS for Medicare, CAQH for commercial payers, and each state’s online portal for Medicaid.
6. Applying During Peak Season
January and July bring the highest volume of new provider applications — hospital systems bring on residents and fellows, practices hire for the new year. Payer staff is overwhelmed and processing slows dramatically. Fix: If possible, schedule credentialing submissions for February–June or August–November.
7. No Follow-Up After Submission
Submitting an application does not mean it is being actively processed. Payers lose documents. Applications sit in queues. Fix: Follow up with every payer every 7–10 business days after submission. Do not assume silence means progress.
8. Applying to Closed Networks
Some payer networks in certain specialties or regions are closed to new providers. Submitting an application to a closed network wastes 60–90 days finding out the answer is no. Fix: Call each payer’s provider relations line before submitting to confirm the network is open.
9. Trying to Manage It Alone
Credentialing is a full-time job that requires constant follow-up, document tracking, and payer-specific knowledge. A practice manager juggling credentialing alongside everything else is a common recipe for delays. Fix: Work with a dedicated physician credentialing service that handles the entire process on your behalf.
What Can Providers Do While Credentialing Is in Process?
This is a question every practice asks — and the answer matters a great deal to your cash flow.
Locum Tenens Arrangements Some practices bring in temporary providers (locum tenens) to cover patient volume while a new permanent provider credentials. The locum credentials under their own existing payer relationships, sees patients, and bills under their own NPI. This is a legitimate strategy for maintaining continuity of care and revenue.
Incident-to Billing In certain clinical situations, a non-credentialed provider can see patients and bill under a supervising physician’s NPI using “incident-to” billing rules. This is only available for specific visit types and has strict documentation requirements. It is not a workaround for credentialing — it is a very specific clinical billing arrangement. Consult your medical billing team before using incident-to billing to make sure you are applying the rules correctly.
Self-Pay and Cash-Pay Patients A provider who is not yet credentialed can still see self-pay patients and collect payment directly. Some practices use this period to build their patient panel with cash-pay appointments, then transition those patients to insurance billing once credentialing is complete.
Important note: Billing insurance under a supervising physician’s NPI for services the supervising physician did not perform — or did not supervise according to payer rules — is a billing compliance violation. If you are unsure what is permitted, talk to your billing advisor before submitting any claims. This is the kind of documentation issue that shows up in a RAC audit.
Recredentialing — What Happens Every 2–3 Years
Credentialing is not a one-time event. Every payer requires periodic recredentialing — typically every 2 to 3 years — to verify that the provider’s credentials are still current and that no new disciplinary actions, license issues, or malpractice claims have occurred.
2026 update: NCQA now requires organizations to monitor provider credentials every 30 days for license expirations, OIG exclusions, medical board actions, and SAM.gov screening. Missing a single monthly check can mean practicing with an expired credential — a compliance violation that creates liability and billing risk.
Building a credentialing calendar that tracks every provider’s recredentialing dates — and sets alerts at 180 days, 90 days, and 60 days before each deadline — is essential for any practice with multiple providers.
Missing a recredentialing deadline does not just mean paperwork. It means your provider’s network participation is terminated until the process is restarted from the beginning — another 90–150 days of delayed billing.

How Pro Health Care Advisors Handles Credentialing for Your Practice
At Pro Health Care Advisors, our physician credentialing service was built specifically for small and individual medical practices — the ones that do not have a credentialing department and cannot afford to have a new provider sitting idle for five months.
Here is exactly what we do:
Document Collection and Verification We gather every required document, verify it for accuracy and currency, and organize it before a single application is submitted. No missing documents. No discrepancies.
CAQH Profile Management We build, complete, and maintain your provider’s CAQH ProView profile — and we track the 120-day attestation cycle so it never lapses.
Multi-Payer Application Submission We submit applications to Medicare, Medicaid, and all commercial payers simultaneously — not sequentially. Parallel submission is the single biggest time-saver in the credentialing process.
Active Follow-Up We follow up with every payer every 7–10 days after submission. We know which payers need nudging, which ones lose applications, and which ones have monthly committee cycles that require timing your submission correctly.
Application Tracking You receive regular status updates on every application. No guessing, no “still waiting to hear back.” You always know exactly where each application stands.
Recredentialing Management We track every provider’s recredentialing dates and initiate the process 120 days before each deadline — automatically, without anyone in your office having to remember.
Hospital Privileging For providers joining hospital medical staffs, we manage the privileging application process alongside insurance credentialing, so both tracks run in parallel rather than sequentially.
We are able to credential providers for all medical plans, Medicare, Medicaid, hospitals, and other facility privileges. Contact us today to discuss your practice’s credentialing needs.
Physician Credentialing Checklist — Start Here Today
Use this checklist before starting any credentialing process. Check off each item before submitting applications.
Provider Documents:
- Current medical license — valid, not expiring within 6 months
- DEA certificate — current and matching practice address
- NPI number (Type 1 — individual provider)
- Board certification certificate
- Medical school diploma
- Residency/fellowship completion documentation
- Complete work history — no unexplained gaps
- CV updated within the last 6 months
- Malpractice insurance certificate — active coverage confirmed
- Complete malpractice claims history
- 3–5 peer references confirmed and willing to respond
CAQH:
- CAQH ProView profile complete
- All documents uploaded as scans
- Profile attested within the last 120 days
- 110-day re-attestation reminder set in calendar
Applications:
- PECOS Medicare enrollment submitted electronically
- Medicaid enrollment submitted in all relevant states
- Commercial payer applications submitted (confirm networks are open first)
- Hospital privileging application submitted if applicable
- EFT setup initiated with each payer
Tracking:
- Credentialing start date logged
- Target approval date set (start date + 120 days)
- Follow-up schedule set (every 7–10 days per payer)
- Recredentialing calendar created with 180/90/60-day alerts
Frequently Asked Questions About Physician Credentialing
Q: How long does physician credentialing take in 2026?
A: Most providers complete credentialing in 90 to 150 days, with Medicare typically being the fastest at 15–30 days for electronic submissions. Commercial payers are the slowest, often taking 90–150 days. Complex situations — multiple states, malpractice history, telehealth across many states — can extend timelines to 180 days or more. The single most important variable is how complete and accurate your initial application is.
Q: Can a physician see patients before credentialing is complete?
A: Yes — but they cannot bill insurance payers for those visits until credentialing is approved. A provider can see self-pay patients immediately. They may be able to bill under a supervising physician’s NPI using incident-to billing rules in specific clinical circumstances. Any billing before credentialing is complete carries compliance risk and should be discussed with your billing team first.
Q: What is CAQH and why does it matter?
A: CAQH ProView is a centralized database that stores provider credentials. Over 1,000 health plans use it as their primary source when reviewing applications. If your CAQH profile is outdated or incomplete, every payer that pulls from it receives wrong or missing information — creating simultaneous delays across all applications. Maintaining a current CAQH profile is one of the most important things a practice can do to speed up credentialing.
Q: What happens if a payer network is closed?
A: If a payer network is closed in your specialty or region, your application will be denied and you will receive a letter saying the network is not accepting new providers. Always call provider relations before applying to confirm the network is open. This saves months of waiting for an answer that was never going to be yes.
Q: How does recredentialing work?
A: Most payers require providers to be recredentialed every 2 to 3 years. The process is similar to initial credentialing but typically faster because the provider is already in the system. Missing a recredentialing deadline terminates network participation, which means the provider cannot bill that payer until a full new application is approved — another 90–150 days. Start recredentialing at least 120 days before the deadline.
Q: What is the difference between credentialing and provider enrollment?
A: Credentialing is the verification of a provider’s qualifications. Provider enrollment is the official registration with a payer that allows billing. Both must happen before a provider can submit claims. Some payers complete both steps in one process; others treat them separately with different forms and timelines.
Q: Can I credential a provider myself without a credentialing service?
A: Yes — but it is one of the most time-consuming administrative tasks in healthcare. Practices that manage credentialing internally typically spend 20–40 hours per provider per application cycle, spread across months of follow-up. For small practices without dedicated administrative staff, this almost always means delays and errors. A professional credentialing service pays for itself when you consider how much revenue a 30-day delay costs.
Q: Does credentialing affect HIPAA compliance?
A: Indirectly, yes. Providers who are not properly credentialed and enrolled can create billing compliance issues that attract audit attention. Maintaining current credentialing is one element of a broader HIPAA compliance and billing compliance program. The two areas of compliance work together to protect your practice from regulatory scrutiny.