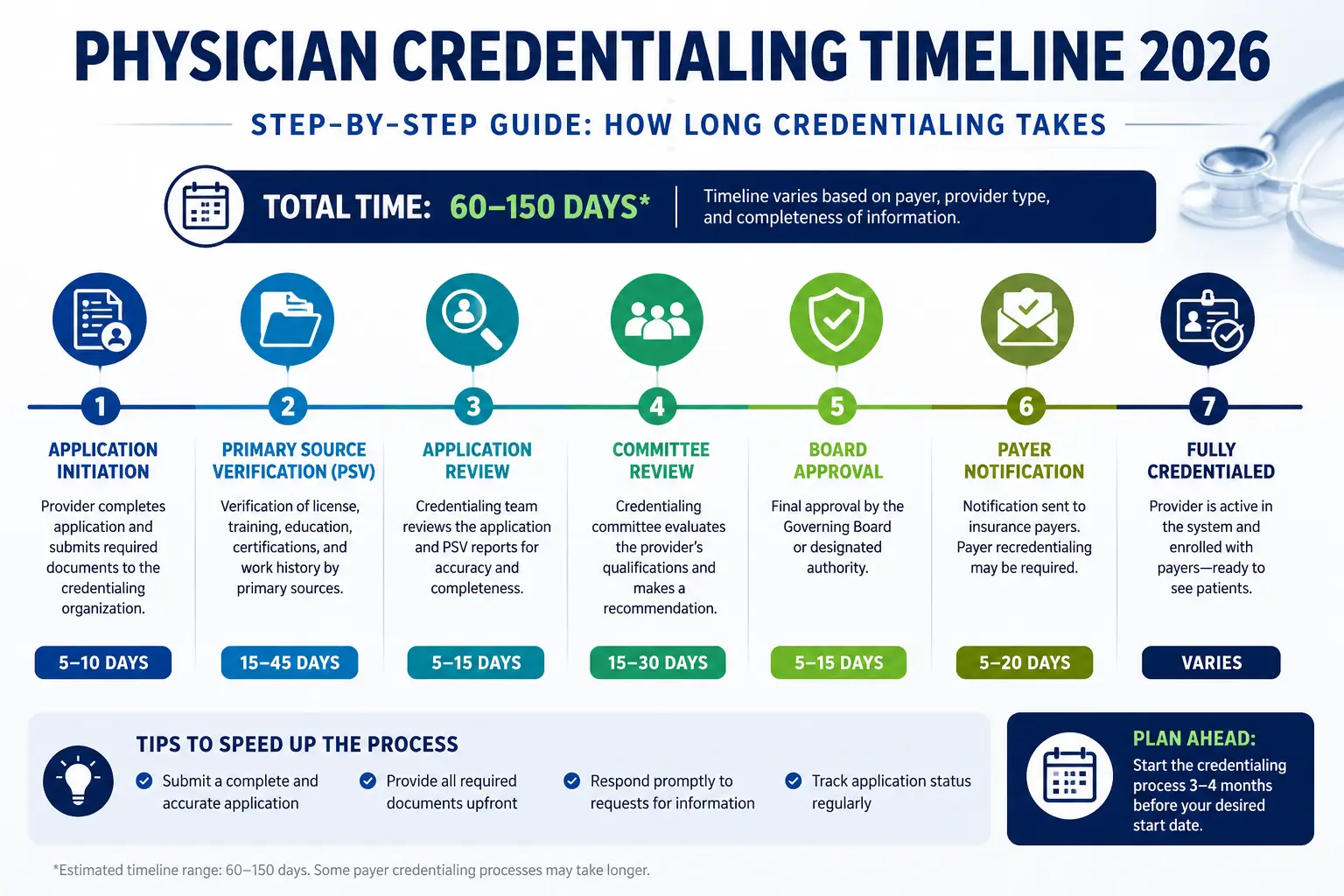
Dermatology medical billing requires accurate CPT and ICD-10 coding, proper modifier usage, payer-specific documentation, and proactive denial management. Because dermatology includes high-volume procedures like biopsies, lesion removals, and Mohs surgery, billing errors can quickly impact reimbursement and compliance. Efficient workflows, clean claims, and specialty-specific coding expertise help dermatology practices improve collections and reduce denials.
Dermatology Medical Billing: Common Coding Challenges and Claim Optimization Strategies
Dermatology medical billing is the process of coding, submitting, and managing insurance claims for dermatology services such as skin biopsies, lesion destruction, excisions, Mohs surgery, and evaluation and management (E/M) visits.
Because dermatology combines office visits with procedural care, billing accuracy directly affects reimbursement, compliance, and claim approval rates.
Voice-search answer:
Dermatology medical billing involves coding skin-related procedures and diagnoses accurately to help providers receive proper insurance reimbursement while reducing claim denials.
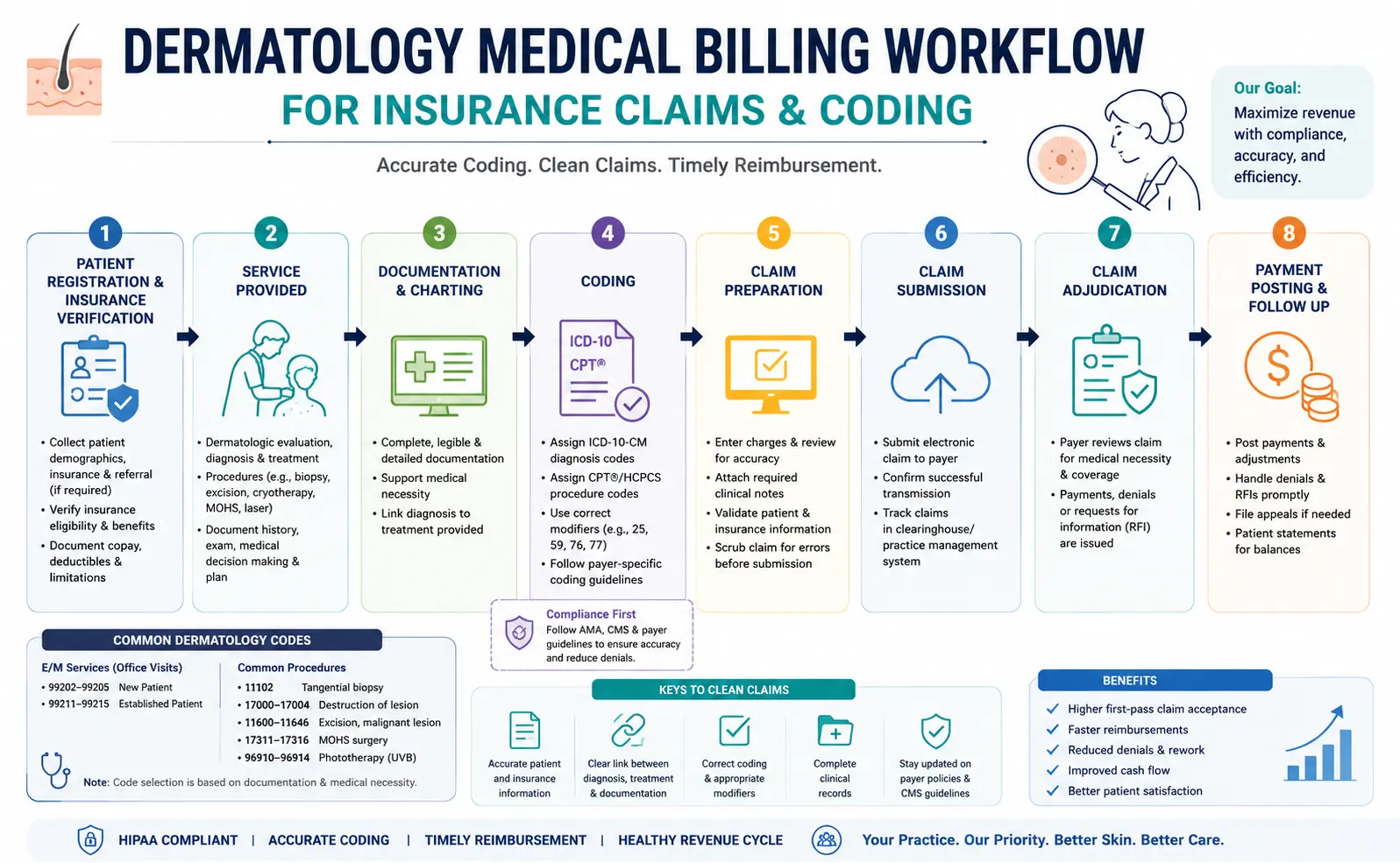
What Is Dermatology Medical Billing?
Dermatology billing includes every financial and administrative step tied to patient reimbursement, including:
- Patient insurance verification
- Prior authorization
- CPT and ICD-10 coding
- Claim submission through clearinghouses
- Payment posting
- Denial management
- Patient billing follow-up
Unlike some specialties, dermatology practices often perform multiple procedures during a single patient encounter. This creates additional coding complexity, especially when modifiers and documentation requirements are involved.
Many dermatology clinics also manage both medical dermatology and cosmetic services, which can create payer classification challenges and patient responsibility issues.
Practices looking to improve operational efficiency often combine specialty billing workflows with broader resources like a “What Is Revenue Cycle Management” guide and a “Medical Billing Process Guide.
Why Dermatology Billing Is More Complex Than General Medical Billing
Dermatology billing involves high procedural volume and strict documentation standards.
Common services include:
- Skin biopsies
- Cryotherapy
- Lesion removals
- Acne treatment visits
- Mohs micrographic surgery
- Phototherapy
- Cosmetic dermatology procedures
Each service may require:
- Specific CPT coding
- ICD-10 medical necessity documentation
- Modifier application
- Prior authorization
- Payer-specific reimbursement rules
For example, using Modifier 25 incorrectly during an E/M visit combined with a procedure can trigger denials or audits.
Approximate insight based on industry patterns: dermatology practices frequently experience denials related to insufficient documentation, incorrect modifier use, and diagnosis-to-procedure mismatches.
Common Dermatology CPT and ICD-10 Coding Challenges
Accurate coding is one of the biggest revenue drivers in dermatology billing.
CPT Coding Complexity
Dermatology procedures often involve nuanced CPT selection.
Examples include:
- Biopsy procedures
- Destruction of benign versus malignant lesions
- Layered closure coding
- Mohs surgery stages
- Multiple lesion counting rules
Incorrect coding can lead to:
- Underpayment
- Claim rejection
- Delayed reimbursement
- Compliance risk
Coders must also understand National Correct Coding Initiative (NCCI) edits and payer bundling rules.
ICD-10 Documentation Requirements
ICD-10 coding must support medical necessity.
For example:
- A benign lesion diagnosis may not justify the same reimbursement pathway as a malignant lesion diagnosis.
- Inflammatory skin conditions may require documentation of severity, location, or recurrence.
Clear physician documentation is essential for accurate claim submission and audit protection.
For a broader understanding of coding relationships, practices often review “Medical Coding vs Medical Billing” educational resources internally.

How Dermatology Claim Submission Works
The dermatology claim workflow follows a structured revenue cycle process.
Step 1: Insurance Verification
Front-desk teams verify:
- Active coverage
- Referral requirements
- Procedure eligibility
- Prior authorization requirements
This helps reduce avoidable denials before the patient visit occurs.
Step 2: Clinical Documentation
Providers document:
- Symptoms
- Diagnosis details
- Procedure notes
- Lesion measurements
- Medical necessity indicators
Strong documentation supports accurate coding and payer compliance.
Step 3: Coding and Charge Entry
Medical coders assign:
- CPT procedure codes
- ICD-10 diagnosis codes
- Applicable modifiers
Charges are then entered into the billing system or EHR platform.
Step 4: Claim Submission
Claims are transmitted electronically through clearinghouses to commercial payers, Medicare, or Medicaid.
Clean claims reduce processing delays and improve first-pass acceptance rates.
Step 5: Payment Posting and Follow-Up
Billing teams reconcile:
- Allowed amounts
- Contractual adjustments
- Patient balances
- Underpayments
Denied claims move into the denial management workflow for correction and resubmission.
Practices often connect this process with a broader “Insurance Claim Submission Process” resource hub.
Denial Management in Dermatology Billing
Denial prevention is a major part of dermatology revenue cycle management.
Common dermatology denial reasons include:
- Missing modifiers
- Invalid diagnosis linkage
- Lack of medical necessity
- Duplicate claim submissions
- Prior authorization failures
- Documentation insufficiency
A structured denial management strategy typically includes:
- Root cause analysis
- Coding audits
- Documentation improvement
- Staff training
- Payer trend monitoring
Many healthcare organizations integrate dermatology denial workflows into larger “How Denial Management Works” operational frameworks.
The Role of Documentation and EHR Systems
EHR and practice management systems play a critical role in dermatology billing accuracy.
Integrated workflows can help:
- Reduce manual entry errors
- Improve coding consistency
- Track prior authorizations
- Flag incomplete documentation
- Automate claim scrubbing
Claim scrubbing tools review claims before submission to identify coding conflicts or payer-specific issues.
HIPAA-compliant systems are essential for protecting patient information during billing and claims transmission.
Best Practices for Improving Dermatology Reimbursement
Use Specialty-Trained Coders
Dermatology coding requires specialty-specific knowledge that general billing teams may lack.
Improve Documentation Specificity
Detailed procedural notes help support medical necessity and reduce audit risk.
Monitor Modifier Usage
Modifiers such as 25 and 59 should be reviewed carefully to avoid payer scrutiny.
Track Denial Trends
Regular denial analysis helps identify recurring workflow problems.
Conduct Internal Coding Audits
Routine audits improve coding accuracy and reduce compliance exposure.
Verify Prior Authorization Requirements
Some dermatology procedures require payer approval before treatment occurs.
What is dermatology medical billing?
Dermatology medical billing is the process of coding and submitting insurance claims for dermatology services such as biopsies, lesion removals, and skin treatments.
Why are dermatology claims commonly denied?
Common reasons include incorrect modifier usage, missing documentation, lack of medical necessity, and diagnosis-to-procedure mismatches.
Which coding systems are used in dermatology billing?
Dermatology billing primarily uses CPT codes for procedures and ICD-10-CM codes for diagnoses.
Does dermatology billing require prior authorization?
Some dermatology procedures and treatments require prior authorization depending on the payer and medical necessity guidelines.
How can dermatology practices improve reimbursement rates?
Practices can improve reimbursement through accurate coding, clean claim submission, denial tracking, documentation improvement, and specialty-trained billing teams.